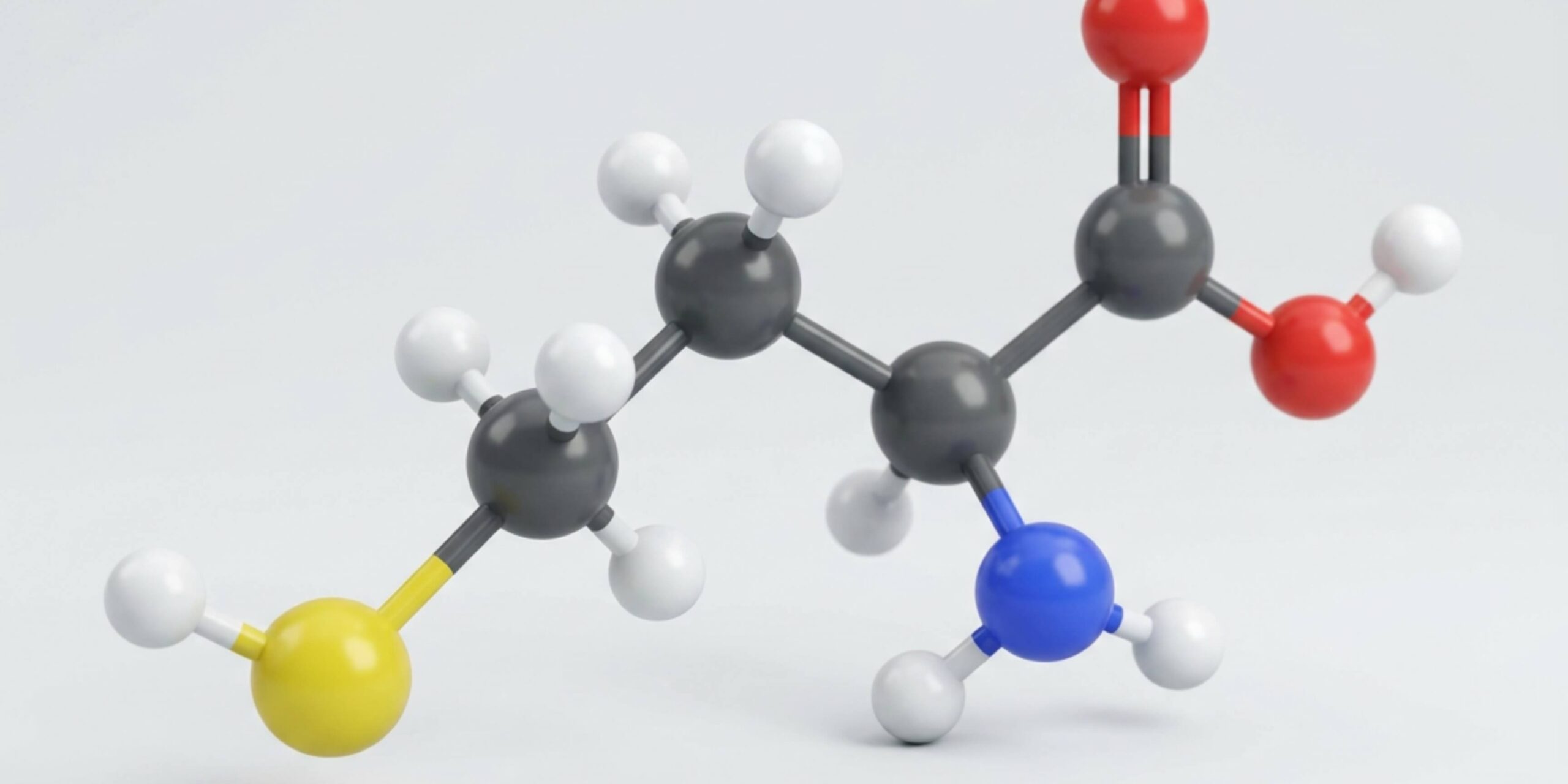
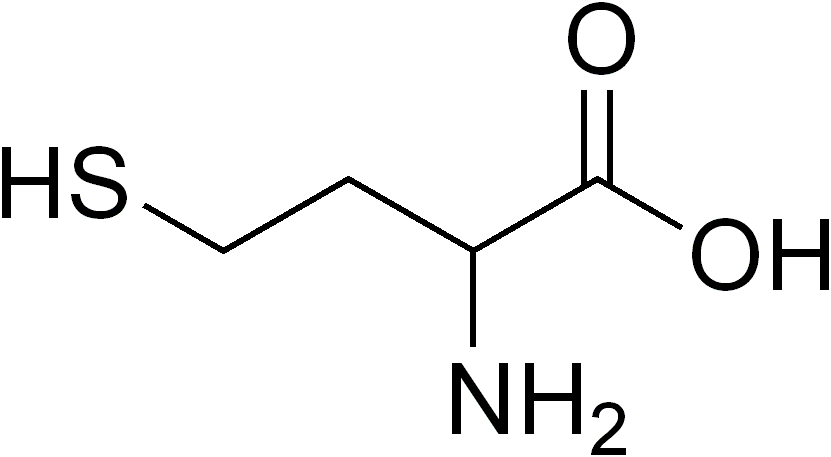
Homocysteine is a naturally occurring amino acid produced during the body’s methylation process. It sits at the centre of key biochemical pathways, including the methionine cycle and transsulfuration pathway, which influence nutrient metabolism, detoxification, and gene expression. To explore these mechanisms in more detail, including how homocysteine affects health and disease risk, read our homocysteine comprehensive overview.
Because homocysteine levels cannot be reliably identified through symptoms alone, many people choose to test their level to understand their risk and take action early.
Under normal conditions, homocysteine is quickly recycled into other useful compounds. This recycling process depends on key nutrients, particularly folate and vitamin B12.
When these nutrients are insufficient, or when the system is under strain, this process becomes less efficient and homocysteine can begin to build up in the bloodstream. A number of factors can contribute to this, including chronic stress, nutrient depletion, higher alcohol intake, and genetic variations that affect how efficiently methylation takes place.[2]
For many people, these influences develop gradually over time and with age, which is why elevated homocysteine can go unnoticed without testing.
High homocysteine levels are most commonly caused by a lack of key B vitamins needed to break it down, particularly vitamin B12, folate, and vitamin B6. These nutrients are essential for methylation, the process your body uses to recycle homocysteine into other useful compounds. When this process is impaired, levels can build up in the blood.
Other factors can also contribute to elevated homocysteine, including genetics, diet, lifestyle, and age. Because these influences are often subtle, many people can have raised levels without obvious symptoms.
Common causes of high homocysteine include:
Because homocysteine is influenced by multiple factors, the only reliable way to know your level is to test it. You can learn more about testing your levels and how to lower homocysteine naturally in the sections below.
If you would like to explore this in more depth, you can read our comprehensive overview of homocysteine metabolism and health or if you’d prefer a visual explanation of how methylation and homocysteine work, watch the short video below.
Elevated homocysteine levels can negatively affect long-term health by promoting inflammation, impairing blood vessel function, and altering gene expression [3,4].
One of its most significant effects is on the lining of blood vessels. Elevated levels can damage this delicate inner layer, reducing flexibility and impairing blood flow throughout the body, including to the brain[3]. Over time, this creates the conditions in which both cardiovascular and neurological diseases can develop.
Large-scale analyses have linked elevated homocysteine to a wide range of health conditions and adverse outcomes: [10]
This breadth of association is not incidental. Homocysteine sits at the centre of several critical biological systems, particularly methylation, vascular health, and inflammation.
For this reason, it is no longer just a marker of risk but actively contributes to the mechanism itself. Elevated levels can actively contribute to vascular damage and brain ageing, rather than just reflect it.
That is what makes it so important.
It is not a diagnostic marker for one specific condition, but a signal that underlying processes in the body may not be functioning as they should.
High homocysteine levels usually do not cause clear or immediate symptoms, so clinicians often overlook them and rarely test for them. It is not a marker of a specific disease. It works more like a warning light, signalling that something in the body is not functioning as it should.
In most cases, clinicians identify it only through testing, often after other health concerns have already begun to develop.
In many individuals, elevated homocysteine is linked to low or poorly utilised levels of key nutrients, particularly vitamin B12, folate, and vitamin B6. When this occurs, some people may experience:
These symptoms are not specific to homocysteine, and they can develop gradually over time. As a result, clinicians often dismiss them or attribute them to stress, ageing, or busy lifestyles; however, they may reflect deeper imbalances in methylation and nutrient status.
You should consider testing your homocysteine levels if you have risk factors for cardiovascular disease or cognitive decline, or if you want a proactive assessment of your long-term health.
Homocysteine levels often rise gradually with age and lifestyle factors, rather than appearing alongside a specific diagnosis. As a result, early testing can help identify elevated levels before symptoms or health issues develop, particularly in individuals at higher risk [5].
Testing may be particularly relevant if you:
Many people are now including homocysteine testing as part of a proactive approach to protecting their brain and long-term health.
A normal homocysteine level is typically below 10 µmol/L, while an optimal level is closer to 7 µmol/L or below. Levels above 10 may indicate increased health risk, and levels above 15 are generally considered high and may require action.
| Level | Range (µmol/L) | Health implications |
|---|---|---|
| Optimal | <7.0 | Lowest risk range and the ideal target for long-term brain and vascular health. |
| Normal (acceptable range) | 7.0 to 10.0 | Generally acceptable, though lower within this range may be preferable for prevention. |
| Moderately elevated | 10.1 to 15.0 | May indicate increased risk and should prompt closer attention to diet, nutrients, and lifestyle factors. |
| High | >15.0 | Associated with elevated cardiovascular and cognitive risk and may warrant testing and targeted intervention. |
Key takeaway: For optimal long-term brain and cardiovascular health, aim for a homocysteine level closer to 7 µmol/L rather than simply staying below the upper limit of “normal”.
Because homocysteine can increase gradually without obvious symptoms, even moderately elevated levels are worth addressing early through diet, lifestyle changes, and targeted nutrients.
Most people with high homocysteine have no obvious symptoms, which means levels can remain elevated for years without being detected. Because of this, testing is the only reliable way to know whether your level is optimal.
Even moderately elevated levels can be worth addressing early, before they contribute to long-term health risks.
Elevated homocysteine levels are strongly associated with cognitive decline, memory impairment, and an increased risk of Alzheimer’s disease, and are now recognised as a modifiable risk factor for dementia [5].
Homocysteine has become a key focus of research into brain ageing. Higher levels have been consistently linked with cognitive decline, memory changes, and increased risk of neurodegenerative conditions such as Alzheimer’s disease [5]. One of the most influential studies in this area is the VITACOG trial, conducted at the University of Oxford.
This study showed that targeted B vitamin supplementation slowed brain atrophy in older adults with mild cognitive impairment, particularly in those with higher homocysteine levels at baseline [8]. In some individuals, the rate of brain shrinkage was reduced by as much as 30 to 50%.
These findings suggest that homocysteine does not merely associate with brain decline but may actively contribute to the processes that drive it.
International consensus statements now recognise elevated homocysteine as a modifiable risk factor for dementia, highlighting the importance of identifying and addressing it early [5].
More detail on this link between homocysteine and dementia is explored in greater depth.
Homocysteine levels can often be lowered through targeted dietary and lifestyle changes, particularly by increasing intake of B vitamins (folate, vitamin B12, and vitamin B6), improving diet quality, reducing alcohol intake, and supporting overall metabolic health.
Before making changes, it can be helpful to test your current level to understand how much support your body may need.
For a more detailed guide, you can explore our article on lowering homocysteine naturally and the role of B vitamins in lowering homocysteine.
Always consult your GP or a qualified practitioner before starting supplementation.
B vitamins are essential for breaking down homocysteine through the methylation cycle.
– Folate from leafy green vegetables and legumes
– Vitamin B12 from animal foods or supplementation
– Vitamin B6 from whole foods such as poultry, fish and bananas
These nutrients are the most important dietary factors for lowering homocysteine.
A balanced, nutrient-rich diet supports efficient metabolism.
Focus on:
– whole foods
– vegetables and fruits
– healthy fats (especially omega-3s)
– adequate protein
Excess alcohol can interfere with B vitamin metabolism and raise homocysteine levels.
– limit intake where possible
– ensure adequate nutrient intake if consuming alcohol
Poor sleep and chronic stress can affect metabolic processes, including methylation.
– aim for consistent, high-quality sleep
– manage stress through lifestyle practices (e.g. exercise, relaxation)
In some cases, supplementation may help support optimal levels.
This may include:
– folate (often as methylfolate)
– vitamin B12
– vitamin B6
Supplementation should ideally be guided by testing and individual needs.
Since elevated homocysteine levels are not usually detected without testing, a blood test is the most reliable way to assess your status.
Testing can be done through your GP or through private laboratory services. Because homocysteine levels are influenced by a wide range of factors, including diet, nutrient status, and genetics, testing provides the only accurate way to understand your individual levels.
For a more complete picture of your brain health, homocysteine is best interpreted alongside other key biomarkers linked to brain and cardiovascular function, including omega-3 status, vitamin D levels, and blood sugar regulation. Assessing these markers together can help identify underlying imbalances that may affect long-term health.
If you choose to test privately, at-home options are available. For example, our at-home homocysteine test provides a convenient way to measure your levels and gain personalised insight into a key driver of brain and cardiovascular health, often before symptoms develop.
You can test it as a standalone marker, or as part of a broader panel such as the DRIfT test, which includes homocysteine alongside other biomarkers relevant to cognitive health.
These tests also contribute to ongoing research into brain health. By taking part, you may not only gain insight into your own health, but also support wider scientific understanding in this area.
Homocysteine is one of the most important markers for long-term brain and cardiovascular health, yet many people don’t know their level.
Because it often has no clear symptoms, testing is the only way to understand your risk and take action early.
By combining testing with targeted nutrition, lifestyle changes, and the right nutrients, it is often possible to bring levels back into the optimal range.
In most cases, yes. Homocysteine is a responsive biomarker, and targeted dietary and lifestyle changes can often improve it.
Optimising the intake and absorption of key nutrients, particularly folate, vitamin B12 and vitamin B6, is central to this process. Adequate omega-3 fats, especially DHA, also play an important role in supporting brain health.
Alongside nutrition, reducing alcohol intake, improving overall diet quality, supporting gut health and managing stress can all help bring levels back into a healthier range.
For those who want more structured support, we guide people through these steps in our 6-month COGNITION brain upgrade programme, available free when you become a FRIEND of Food for the Brain.
With appropriate dietary and lifestyle changes, homocysteine levels can often improve within a few weeks to a few months, depending on the underlying cause and consistency of intervention.
Testing is particularly relevant for anyone taking a preventive approach to long-term health, and our tests are suitable from age 2 onwards.
It may be especially useful for those with risk factors for cardiovascular disease or cognitive decline, low B vitamin status, or symptoms such as fatigue, brain fog or low mood.
Because homocysteine levels can rise silently over time, many people with elevated levels would not otherwise know without testing.
If you would like to check your levels, you can order a simple at-home blood test.
A biomarker is a measurable substance in the body that provides insight into how well specific biological processes are functioning. Homocysteine serves as a biomarker because it reflects how efficiently key systems operate, particularly methylation, nutrient status and vascular health.
Unlike many markers that relate to a single condition, homocysteine offers a broader view of the underlying processes that influence both brain and cardiovascular health.
For long-term health, “normal” is not the same as optimal.
Levels below 10 µmol/L are generally associated with lower risk. For a more preventive approach, aiming for 7 µmol/L or below is often recommended as a more protective target for brain and cardiovascular health.
Levels above this range may indicate that the body is not processing homocysteine efficiently and could benefit from targeted nutritional and lifestyle support.
Elevated homocysteine increases the risk of several chronic conditions, particularly cardiovascular disease and cognitive decline. Research also suggests it may contribute to underlying processes such as inflammation, oxidative stress and damage to blood vessels.
It is not a diagnosis in itself, but a useful signal that something in the body may require attention.
Food for the Brain offers a convenient at-home, finger-prick homocysteine test designed for high analytical accuracy. Traditionally, clinicians have measured homocysteine using a venous blood sample, which requires rapid processing and centrifugation.
In partnership with our laboratory team, we have developed a method to stabilise the sample, helping to ensure reliable results while making testing more accessible.
You can measure your levels using the Food for the Brain Homocysteine (HCY) test, or as part of the DRIfT test, which includes a broader range of biomarkers linked to brain health.
Further details on the validation of this method can be found in our homocysteine blood test validation document.